Table of Contents
Toggle
Hashimoto’s Immune Function: Ending the “Wait and See” Era
Recent breakthroughs in Hashimoto’s immune function are reshaping how doctors understand this autoimmune thyroid condition. The 2025 Nobel Prize discoveries reveal how the immune system controls thyroid attacks, offering hope for earlier and more effective interventions.
Understanding Hashimoto’s: The Autoimmune Fire
Hashimoto’s thyroiditis isn’t just a hormone deficiency—it’s an active autoimmune condition. That means the immune system is aggressively targeting your thyroid, which can cause hormone levels to fluctuate throughout the day. To understand the full picture of Hashimoto’s disease and how immune regulation affects thyroid health, you can read our detailed guide on Hashimoto’s Thyroiditis: Symptoms, Causes, and Treatment.
People with Hashimoto’s may notice:
- Fluctuating energy and fatigue: Some days feel normal, other days completely drained.
- Brain fog or trouble remembering things: Tasks that were easy before can suddenly feel overwhelming.
- Anxiety or sadness: Mood shifts, nervousness, or low spirits can appear when hormones are unstable.
- Muscle soreness and tightness: Stiffness, aches, or discomfort in muscles and joints.
- Hair thinning: Often visible at the outer edges of the eyebrows, a common sign of thyroid stress.
- Neck swelling or goiter: Noticeable enlargement in the thyroid area.
Quick fact: Because these symptoms often overlap with general hypothyroidism, many people are misdiagnosed or treated only with thyroid hormone replacement—without addressing the autoimmune aspect.
Limitations of Standard Thyroid Therapy
Right now, most doctors treat Hashimoto’s as if it’s straightforward hypothyroidism: they check your labs, prescribe levothyroxine (T4), and adjust doses to get your numbers in range.
While this approach addresses hormone deficiency, it doesn’t calm the immune system. Even if your lab results look “normal,” the autoimmune attack can continue quietly, which is the core of the “wait and see” dilemma
Important Note: Effective care should include both hormone support and strategies to modulate the immune system, protecting your thyroid over the long term.
Nobel Prize Insights on Autoimmunity
In 2025, Mary E. Brunkow, Fred Ramsdell, and Shimon Sakaguchi received the Nobel Prize in Physiology or Medicine for uncovering how the body naturally prevents autoimmune attacks—a process called peripheral immune tolerance.
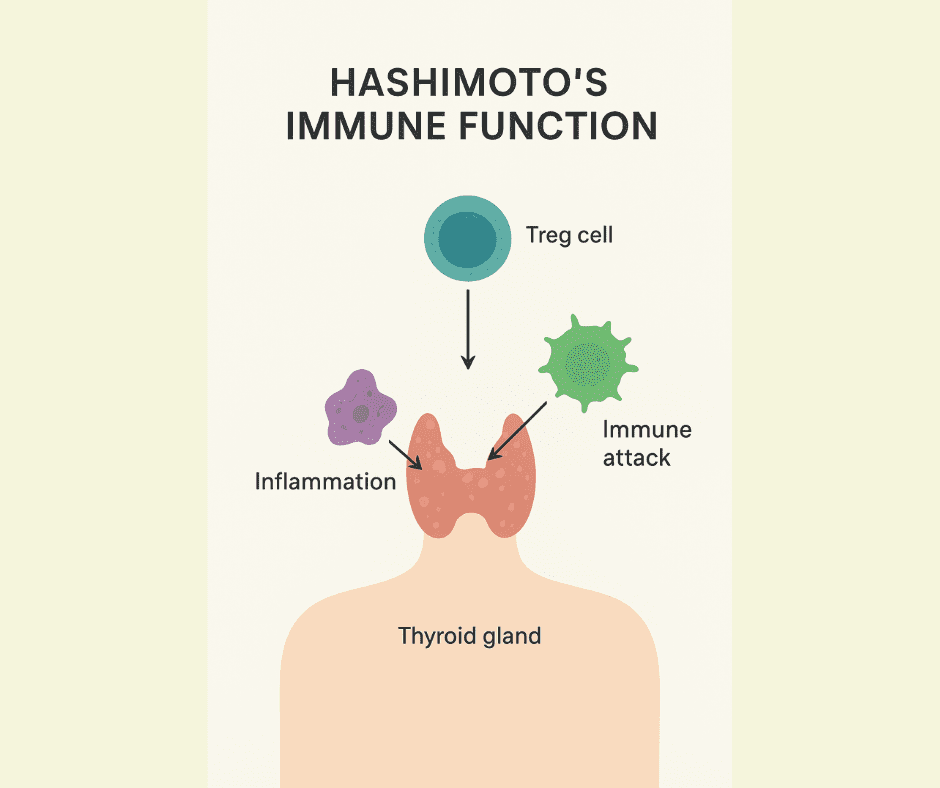
At the heart of this process are regulatory T cells (Tregs), often called the “security guards” of the immune system. They prevent the immune system from attacking your own tissues while still defending you against infections.
The researchers also discovered the FOXP3 gene, which controls Treg development. Mutations in FOXP3 can lead to serious autoimmune diseases, highlighting the importance of these cells for immune balance.
Did you know? Boosting Treg function is a promising approach for managing autoimmune conditions like Hashimoto’s because it helps the body restore its natural tolerance.
Supporting Immune Regulation in Hashimoto’s Immune Function
Building on these Nobel discoveries, there are practical ways to support Treg function and reduce the strain on your immune system. This goes beyond simply replacing hormones—it aims to calm the autoimmune attack at its source.
1. Diet: Reduce Inflammation & Support Hashimoto’s Immune Function
What you eat directly affects both your immune system and thyroid function. An anti-inflammatory, nutrient-rich diet can help protect thyroid tissue and promote immune stability:
- Gluten-free & dairy-free: Many with Hashimoto’s react to these foods, which can trigger immune flares.
- Whole, organic foods: Vegetables, leafy greens, colorful fruits, and legumes provide antioxidants to fight oxidative stress.
- Quality proteins & fats: Grass-fed meats and omega-3-rich wild-caught fish reduce inflammation.
- Stabilize blood sugar: Include protein, fiber, and healthy fats at each meal to avoid insulin spikes that can worsen inflammation.
- Limit processed foods & refined sugar: These can disrupt your gut and drive chronic inflammation.
2. Reduce Toxin Exposure
Environmental toxins can provoke autoimmune activity by overloading the immune system. Consider:
- Water filters: Reduce chlorine, fluoride, and heavy metals.
- Low-toxin products: Swap conventional cleaning and beauty products for natural alternatives.
- Avoid plastics: Store food in glass or stainless steel to minimize hormone-disrupting chemicals.
- Minimize pesticides: Choose organic produce when possible.
3. Key Nutrients for Thyroid & Immune Support
Certain vitamins and minerals are essential for thyroid hormone production and immune balance. Testing your levels before supplementation ensures safety and effectiveness:
- Selenium: Supports hormone synthesis and regulates autoimmunity (Brazil nuts, seafood, eggs)
- Zinc & Copper: Important for immune cell function; balance is key
- Vitamins D & B12: Support energy, immunity, and hormone activity
- Glutathione: A powerful antioxidant that protects thyroid tissue
- Omega-3 fatty acids: Reduce inflammation and support Treg function
4. Lifestyle & Stress Management
Chronic stress can fuel autoimmune activity. Prioritizing lifestyle changes helps calm an overactive immune system:
- Restorative sleep: Aim for 7–9 hours nightly to support hormones and immunity.
- Stress-reducing practices: Meditation, yoga, deep breathing, and mindfulness can lower inflammatory stress hormones.
- Gentle exercise: Walking, swimming, or yoga supports circulation without overtaxing your body.
- Address emotional trauma: Therapy or support groups can help soothe the nervous system and reduce autoimmune triggers.
5. Medical Options to Consider
While diet and lifestyle are essential, some patients may benefit from targeted treatments:
- Thyroid hormone replacement: restores hormone levels. Some benefit from combination therapy (T4+T3)
- Low-dose naltrexone (LDN): Emerging therapy that may reduce autoimmune inflammation
- Gut health restoration: Healing intestinal permeability and balancing the microbiome can reduce triggers for autoimmunity
The Takeaway: Supporting Hashimoto’s Immune Function
Early testing for thyroid antibodies (TPOAb, TgAb) is important for understanding the role of Hashimoto’s immune function. From there, combining strategies—such as eating anti-inflammatory foods, reducing stress, supporting nutrients, and exploring medical options when needed—can make a noticeable difference. The focus isn’t just on lab results; it’s about feeling healthier, having more energy, and keeping your thyroid safe for the future.
References
- Brunkow ME, Jeffery EW, Hjerrild KA, Paeper B, Clark LB, Yasayko SA, Wilkinson JE, Galas D, Ziegler SF, Ramsdell F. Disruption of a new forkhead/winged-helix protein, scurfin, results in the fatal lymphoproliferative disorder of the scurfy mouse. Nat Genet. 2001;27:68-73.
- Wildin RS, Ramsdell F, Peake J, Faravelli F, Casanova JL, Buist N, Levy-Lahad E, Mazzella M, Goulet O, Perroni L, Bricarelli FD, Byrne G, McEuen M, Proll S, Appleby M, Brunkow M. X-linked neonatal diabetes mellitus, enteropathy and endocrinopathy syndrome is the human equivalent of mouse scurfy. Nat Genet. 2001;27:18-20.
- Bennett CL, Christie J, Ramsdell F, Brunkow ME, Ferguson PJ, Whitesell L, Kelly TE, Saulsbury FT, Chance PF, Ochs HD. The immune dysregulation, polyendocrinopathy, enteropathy, X-linked syndrome (IPEX) is caused by mutations of FOXP3. Nat Genet. 2001;27:20-21.
- Hori S, Nomura T, Sakaguchi S. Control of regulatory T cell development by the transcription factor Foxp3. Science. 2003;299:1057-1061.
- Caturegli P, et al. Hashimoto’s Thyroiditis: Clinical Features and Autoimmune Mechanisms. N Engl J Med. 2014; 371:993-1004.
- Weetman AP. Autoimmune Thyroid Disease: Propagation and Management. Lancet. 2012; 379:1141-1152.
- American Thyroid Association (ATA). Guidelines for the Management of Thyroid Disease. https://www.thyroid.org/professionals/ata-professional-guidelines/
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). Hashimoto’s Disease Overview. https://www.niddk.nih.gov/health-information/endocrine-diseases/hashimotos-disease
- Cleveland Clinic. Thyroid Antibodies Testing. https://my.clevelandclinic.org/health/diagnostics/thyroid-antibodies
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) – Hashimoto’s Disease
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) – Hashimoto’s Disease